South County Health, a small nonprofit system in bucolic southern Rhode Island, owes a large part of its success to its ability to manage transitions of care – an increasingly urgent imperative as healthcare moves from fee-for-service to value-based reimbursement.
The system’s flagship is South County Hospital, a 100-bed community hospital. The system also includes South County Home Health Services (a home health agency); South County Surgical Supply (home medical supplies); South County Medical Group, with 65 physicians and advanced-practice providers, and two Medical and Wellness Centers, one in Westerly and the other in East Greenwich, with urgent-care facilities and an array of primary-care and specialist physicians.
South County Hospital has long had very high marks for quality and patient satisfaction. Indeed, surveys have often called it the best hospital in its state and one of the best in New England. It was recently awarded a five-star rating by the Hospital Consumer Assessment of Healthcare Providers and Systems (HCAHPS), putting it in the top 2 percent of those surveyed nationwide.
Louis R. Giancola, the system’s president and chief executive, attributes much of the hospital’s success in patient satisfaction — and fiscal stability — to the strong engagement of its staff, which “we keep in the know’’; a “supportive board’’; the long-term loyalty of people in the service area, and the “nimbleness of a community hospital’’. Having a relatively affluent market with many well-insured people hasn’t hurt either, he acknowledged.

Mr. Giancola.
A particular point of pride is: “We’re good at transitions of care. Maybe that’s a result of our being small.’’
South County Hospital, like virtually all health systems these days, faces many challenges in dealing with the rewards and penalties involved in the forced-march transition to value-based reimbursement. Mr. Giancola notes:
“Medicare incents us to improve patient satisfaction, reduce hospital infections and avoid various patient injuries. Most commercial payers (insurers) have followed suit. I believe the threat of reduced payments has focused our attention on these measures even though we sometimes complain that the measures are not always fair.’’ (See below.)’’
“It’s all about blocking and tackling. The biggest issue is readmissions within 30 days. {South County has long had lower readmission rates than most hospitals.} We’ve really focused on managing the transition from the hospital to another level of care. The important element is good communication between the hospital providers and the skilled-nursing facility, home health and the doctors caring for the patients in the community.’’
Part of South County’s recognized success in overseeing clinically successful and financially efficient transitions – and, in so doing, reducing costly readmissions — has been its emphasis on using, when possible, home health care instead of nursing centers to save money and improve care, Mr. Giancola said.
The Centers for Medicare & Medicaid Services and other regulators and payers have been pushing hard for better patient-care management, especially since the Affordable Care Act took full effect. Much of South County Health’s work in this area involves helping primary-care physicians to be better traffic managers of their patients’ care.
Another transition success story he cites is medication reconciliation. “Often patients are confused about their drugs and that can lead to readmission because they take drugs that are contra-indicated or they take two meds designed to address the same problem. We’ve hired pharmacists that review meds in the hospital to ensure they are reconciled and the patients get clear advice on discharge.’’
He notes as an example of what might sometimes be unfair pressure from the Feds: CMS’s making hospitals put many patients who have to stay in the hospital for a night or two into “observation’’ status instead of as inpatients, thus slashing potential hospital reimbursement.
Bundled payments, Medicaid and an ACO
An increasingly important strategy for controlling costs and improving care is bundled payments.
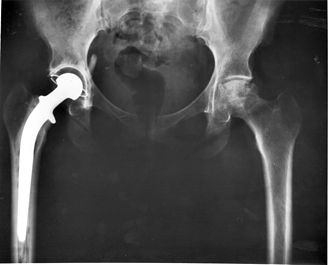
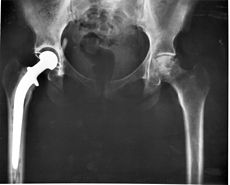
South County Health participates in a bundled-payment program for joint-replacement patients with Blue Cross for their Medicare Advantage and commercial-insurance members. (Cambridge Management Group has been doing a lot of work in bundled-payment programs and so this particularly caught our eyes.)
With older-than-average market demographics, the joint-replacement business is a major contributor to the system’s bottom line. (However, while the system is financially stable, its operating margin is only about 2 percent; the system is closely managed.)
Mr. Giancola said that, as with many things in the brave new world of value-based medicine, it’s unclear what sort of savings may come out of the move to bundled payments. However, he thinks that the clinical benefits are clear:
“The bundling process helps us to get a better handle on the clinical process. Having to report quality throughout the entire episode of care makes for better transitions and final outcomes.’’
South County Hospital’s leaders are happy that the Affordable Care Act has put so many uninsured people into Medicaid. While Medicaid reimbursements lag those of Medicare it’s a lot better than no insurance for low-income people. Many of those people, of course, have long used the emergency room as their major source of “free’’ (to them) medical care.
But, perhaps surprisingly, Mr. Giancola told us, Medicaid expansion has not yet cut the flow of people into South County Hospital’s ER, despite efforts encouraged by public and private insurers to promote more and better preventive care to keep people out of the ER. “ERs are too handy for lots of people,’’ he observed.
South County Hospital has had to deal with many other changes, whose long-term fiscal effects are difficult to predict. One is the rising number of employed physicians, hired, Mr. Giancola says, to ensure that the hospital can maintain the range of services that patients want and need in an acute-care facility, such as obstetrics.
Mr. Giancola notes that’s expensive. “Hiring doctors away from private practices to be based in the hospital puts them in more expensive places, with expensive support staffs, equipment and technology. The jury is out on whether the increase in hospital-employed physicians will save money in the long run.’’
Also unknowable at this point is whether South County’s participation in an Accountable Care Organization with Blue Cross & Blue Shield of Rhode Island (BCBSRI) and Integra Community Care Network will ultimately save money. Integra is a partnership of Care New England Health System and its network physicians, Rhode Island Primary Care Physicians Corporation and South County Health and its network physicians. Focused on population-health management, the ACO provides incentives for Integra’s providers to proactively manage patient health, with a heavy emphasis on prevention of illness, while trying to restrain costs.
South County Health, as befits a, well, beloved local institution is big on promoting community-wide collaboration of institutions that can help improve not just healthcare in a clinical sense, but population health.
Toward that end, it has brought together such diverse agencies as the YMCA, the five Federally Qualified Health Centers in its area, school systems, the local Community Action Program and community members to harness the resources of the community. Whatever happens to the ACA, the move toward community and population health will continue, and South County Health will help lead it in southern Rhode Island.
Mr. Giancola has written: “Our long-term goal is to inspire the broader community to see health as a community issue and to mobilize government, schools, businesses and citizens at large to rally around efforts to ensure a healthy community.’’