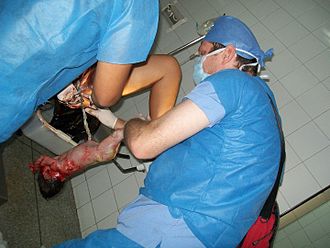
Assisting in childbirth.
The federally affiliated Health Care Payment Learning and Action Network (HCPLAN), looking to advance value-based care and save payers money, advocates using bundled-payment systems to address the high-volume admissions related to maternity and newborn care. As well it would: Maternal and newborn stays together represent more than 20 percent of all hospital stays, says the Agency for Healthcare Research and Quality.
HCPLAN is a public-private collaborative network trying to reach the federal government’s goal that 50 percent of all healthcare payments be via alternative (value-based) payment models by 2018. The network’s clinical-episode payment work group has named maternity care, elective knee and hip replacement and coronary-artery disease treatment (mostly involving bypass surgery) as priorities for episode-based payments.
Work group members see many ways to improve care and cut costs in maternity and newborn care. Consider that the U.S. cesarean-section rate is high — more than 30 percent of births, says the World Health Organization — despite the expense and potential danger to mother and baby. Cesarean deliveries are lucrative for physicians and hospitals.
Further, more than 9 percent of births are pre-term, including many early elective deliveries, which of course means more neonatal intensive care. All this with U.S. infant-mortality rates higher than in most of the Developed World.
As Hospitals & Health Networks reports, Geisinger Health Plan, in central Pennsylvania, has used bundled payments approach for obstetrics for six years — and with good results, John B. Bulger, D.O., Geisinger’s chief medical officer for population health, told H&HN.
“Early elective deliveries almost immediately dropped to zero when the obstetrics department started to focus on processes of care. That resulted in fewer C-sections and reduced NICU use. ‘It is a win-win-win because the baby is healthier, happier, the mother is healthier and happier, and the population is healthier and happier because it is less costly to the system,’ he says.”
“Geisinger’s perinatal care bundle, available only for low-risk pregnancies, includes all prenatal, labor and delivery, and postpartum care for the mother only; the baby’s care is not covered in the bundle.”
H&HN says that “despite Geisinger’s success, its particular approach has not been widely adopted. A handful of payers and health systems are experimenting with maternity care bundles, but most are waiting for somebody else to figure out best practices. The first challenge is the sheer length of the episode.”
‘We feel pretty strongly that an episode should include prenatal, postpartum and — ideally — 30 days of newborn care,” Brynn Rubinstein, senior manager for Transform Maternity Care at the Pacific Business Group on Health, told H&HN. “It’s really hard to navigate all of the providers that a woman and baby might see, and all of the other conditions related to pregnancy, or unrelated to pregnancy, and how to include those in the episode.”
”Rubinstein, who is working with plans and purchasers to implement the recommendations outlined in HCPLAN’s white paper on maternity care episode payments, says purchasers are tired of the variation in cost and quality of maternity and newborn care.”
‘“While there are many obstacles to navigate, they are all challenges that can be overcome. It may take a few years, but they can absolutely be overcome, and we need to start today.”