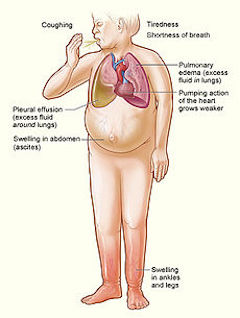
Signs of heart failure.
Geisinger Health System, based in Danville, Pa., has long received attention for its advances in integrated care. Now a piece in NEJM Catalyst says it has used better care integration to improve medication management and reduce emergency-room visits.
FierceHealthcare reports that Geisinger started to consider every unplanned admission for acute heart failure that required only diuretic therapy for treatment as something to be avoided. System leaders then developed a “central urgent heart failure clinic, offering onsite review of each patient’s care plan, coordination between nurse navigators and community nurse case managers, and medication management.”
The NEJM Catalyst piece summed up the findings thus:
-
“High-quality, integrated, multidisciplinary teams can be organized around heart-failure care.
-
“Heart-failure clinical experts can effectively disseminate, implement, and monitor care plans through community partnerships with nurse case managers.
-
“A unified approach to assessing heart-failure cases through the electronic medical record, by phone, and during face-to-face encounters helps to integrate the work of multidisciplinary teams.”
Preliminary data indicates that the new approach saved the system $240,000 in ED visits in 2015, with 28 percent of hospitalized heart-failure patients avoiding emergency care. Meanwhile, monitoring of renal function and potassium rose to 80 percent from 41 percent.