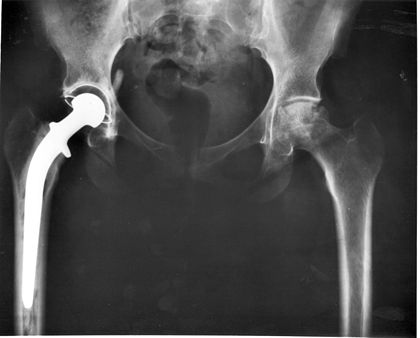
See hip replacement at left.
David Blumenthal, M.D., and David Squires have written a very cogent and realistic overview of the promises and pitfalls of bundled payments. Among their remarks:
“Healthcare economists are drawn to bundled payments because a bundle of care constitutes a clinically and intuitively meaningful “product” — in this case, the clinical episode. Defining clear products in healthcare helps create markets in which providers directly compete on quality and price. One barrier to effective healthcare markets has been that prices, when available, tend to relate to inputs into clinical care — such as pills, bandages, bed days, or X-rays — that are not meaningful to consumers of care and that don’t necessarily predict the total costs of care. ”
“Yet bundled payments have drawbacks. First, it can be complicated to define and track the type of care that should be included in the bundled payments for which a given provider is at risk. Knee and hip replacements are well-suited to bundles because they often involve comparatively young patients who are physically active (often the source of their joint damage) and want to remain so. But when patients have multiple chronic conditions that interact with each other, it becomes less clear whether the bundle should include the costs of caring for all those problems….Monitoring the fairness of these interactions could become burdensome and increase administrative costs.”
“{A}s the hip patient example suggests, bundles could inhibit certain types of care coordination, even as it encourages other types. On the plus side, bundles may encourage hospitals to work more closely with rehab centers. On the negative side, bundles may encourage specialists’ already strong tendency to see patients not as whole individuals, but as single disease problems or procedures, and to diminish their sense of responsibility for costs of illnesses not included in their particular bundled payment.”
{B}undled payments could encourage destructive competition for patients with profitable bundles. The otherwise healthy patient needing a knee replacement may prove more profitable than a knee replacement patient with complicating problems such as heart, lung, or kidney disease. While risk adjustment could somewhat compensate for cherry-picking, such adjustments have not proven foolproof in the past, and an entirely new fleet of risk adjusters that are specific to given clinical episodes will likely be required. Monitoring the work of multiple risk adjusters and possible gaming by providers could become yet one more administrative expense.”
“{B}undled payments may make it harder for population-based payment methods like ACOs to be successful. Providers who participate in ACOs assume responsibility for all the care their patients need during a given period of time, including specialty care. This general accountability for their patients’ health encourages efforts to coordinate care, especially for complex patients. Still, to be financially viable, ACOs must generate savings from existing services. If independent specialty providers capture the elective procedures for which savings are easiest to generate through bundled payments, it could be harder for ACOs to find those savings within their own service mix.”
To read this entire essay, please hit this link.





